![]()
by Fred Lanphear
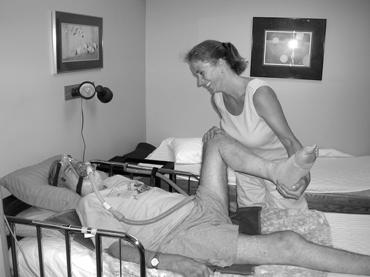
Michelle Grandy doing weekly stretching exercise with Fred.
December 2007 brought about a huge change in my life!
I received a diagnosis of ALS, better known as Lou Gehrig’s Disease. ALS is a fatal disease without any known cure; the life expectancy averages two to five years after diagnosis. It was about this time Songaia Cohousing Community began the 10-week course Aging in Place Successfully, which explores the notion of community providing a place to live until death. I was to be a “guinea pig” for the concept of aging in place, as ALS is a degenerative disease that can be cared for at home, but does require an intensive, shared care structure as the disease progresses. I requested a community circle in January 2008 to share my diagnosis with everyone and to ask for their support as I move into the last phase of my life.
Songaia is a multigenerational cohousing community located in Bothell, Washington. It has 10.7 acres of wooded hillsides, orchards, gardens, and meadows, in the suburbs 20 miles northeast of Seattle. We are 15 families — 34 residents, consisting of nine children, 16 adults (ages 30-59), and eight seniors (over 60). The community is nine years old and has not experienced any deaths.
During the sharing circle I offered an image of my condition as an adventure and invited the community to be a part of that adventure, “’til death do us part.” I asked folks to come and sit with me for sharing stories, a form of support that really appeals to me. Although it is noted that in a more final stage of ALS, one could be unable to speak, singing or reading poetry would be most appropriate as it would not require a response except with a smile or blinking of my eyes. Other types of support included physical care, in the form of bodywork (yoga therapy, stretching, and massage), equipment and house modification (door removal and ramp installation) and upkeep. Others have helped with my writings — a book about Songaia, my memoirs, and a journal of my journey with ALS.
As recommended in the course on aging, a “Share the Care” team formed, with Jean, Karly, Marilyn, and Carol volunteering to “captain” the contributions and care from the community as well as family members and friends. The team designed a survey and sent out emails. Although the larger community care began later on, folks at Songaia began immediately to provide support. They installed grab bars in the shower and platforms on a lift chair and commode, helped lift me out of chairs, and visited me often, with hugs and great conversations, throughout the year. They also responded to my wife Nancy’s emergency calls for help when as I was precariously suspended while trying to get out of the car seat or when I fell off my scooter seat while trying to get off of it. I carried a cell phone programmed to be able to call various community members by pressing a single digit.

Barbara Bansenauer and son Ian hoisting Fred out of his chair
in preparation for helping to get into bed.
A little over a year after my diagnosis, I had a fall and broke my ankle. This shifted me into a new level of care. I could no longer walk and required assistance getting from a wheelchair into bed. A Hoyer lift and hospital bed were obtained for this purpose. It could be operated by one person but it was easier with two. Each Monday evening at dinner the care coordinator would pass a sheet of paper for people to sign up to help put me to bed for the week; it was called the “Tuck-in-Fred” team. Often an older child would come with a parent to help. Bedtime included helping me do leg exercises and goodnight hugs after I am in bed.
Three community women offered to work with me on a weekly basis to provide bodywork to keep my joints limber. Cindy does yoga therapy twice a week, Jean does a full body massage, and Michelle an active body exercise each week. Other folks came occasionally for massage and exercises. Passive exercise is crucial, as I sit in a wheelchair all day. During the day community members, including the kids, will help me exercise/stretch my legs while I am still in the chair. When I was able to go to the swimming pool, Brent or Carol would come with Nancy to help me get in and out of the pool.
Periodically a care circle is held when there is a change in my health status and a new level of care is required. Medicare, plus our Group Health insurance, covers home health care and sends out a specialist as needed. For example, when I needed help to transfer from my chair to the bed or another chair, a physical therapist came and trained Nancy and about 12 community members how to move me using a transfer board.
Visits by community members to provide physical care are often used as an opportunity to check in with me about my spiritual state of being. These may be brief check-ins or lengthy discussions. They are opportunities to provide emotional support as well as knowledge about how best to care for me. Karly, a speech therapist and neighbor, visited often, but about once a month she also checked in on my breathing, swallowing, and how often I might have had choking issues.

Cyndi Kershner doing her weekly yoga therapy session with Fred.
The community decided to celebrate my life while I was still able to enjoy it and before I died. The first challenge was to create a context for the celebration. We decided it was not a living funeral or an early 80th birthday celebration. Instead, it would be a rite-of -passage ceremony marking my transition from an active elder to a “revered grandfather,” one who tells stories and shares his wisdom. To symbolize my new role, our grandchildren, along with the community children, enveloped me with a blanket in the form of a Grandfather robe! It was a grand celebration with 130 attendees. Individuals were invited to share their memories and good wishes to me. Once again I felt blessed, honored, and cared for so deeply.
The community does not see this care as an obligation but rather as an opportunity to be a part of my journey. Our family provides the primary care and integrates homecare from our health care providers along with support provided by the ALS foundation. Individual members of the community have stepped forward to take on the responsibility of coordinating the “Share the Care” team that includes family members, friends, and community members. This distributes the workload so that it does not become a burden to just a few. This arrangement works. It might not work as well if I had an illness with more serious complications, as in the dementia of an Alzheimer patient. Each situation has to be considered based on the needs and capability of the community. I have come to realize that I couldn’t have picked a better place to be in my condition.
These past two years have brought about huge changes in our community of Songaia! These changes have given us opportunities and possibilities for new relationships and connections with each other. We have all become more present to the priceless experience of daily living, even death and dying.
 Fred Lanphear has lived in various forms of intentional community for over 35 years. He is a cofounder of Songaia Cohousing near Seattle, where he currently lives and where he was initiated as an Elder in 2006. Fred was a cofounder of NW Intentional Communities Association (NICA) and serves on its Board of Directors. He also served on the Fellowship of Intentional Communities (FIC) Board for two terms.
Fred Lanphear has lived in various forms of intentional community for over 35 years. He is a cofounder of Songaia Cohousing near Seattle, where he currently lives and where he was initiated as an Elder in 2006. Fred was a cofounder of NW Intentional Communities Association (NICA) and serves on its Board of Directors. He also served on the Fellowship of Intentional Communities (FIC) Board for two terms.










While there are many positive aspects of what Fred discusses here, the truth of the matter is that this thing called als is just a nerve health problem that he could have solved. So the whole terminal disease thing is not really right.
To understand how and why the type of neurodegeneration commonly called als happens, and to learn about solving the problem and healing, see my work, along with the work of Gabor Mate, Craig Oster, Steven Shackel, Dean Ornish, Bruce Lipton, David Atkinson and Evy McDonald.